What Are Probiotics Benefits? 11 Signs You’re Deficient and What to Do About It

What are probiotics good for?
Hippocrates is famous for saying, “All disease begins in the gut.”
2500 years later, science is proving how right he was.
Thousands of studies link an unhealthy gastrointestinal tract to an increasing number of physical and mental diseases, including diabetes, depression, and even Parkinson's disease and cancer.
[Say bye-bye to your digestions issues for good! Our 3-in-1 for Total Gut Health is our Deal of the Month. Save up to 25% off today.]
In this article:
- What Are Probiotics Good For?
- What Are Probiotics?
- How Do You Know You Have Enough Good Bacteria?
- Do You Need Probiotics?
- How Do You Get Enough Probiotics?
Probiotic Benefits for Your Health
What Are Probiotics Good For?
We’re learning that a healthy balance of “good” gut bacteria relative to the bad ones is critical to well-being in more ways than we’ve ever known.
And the key to that balance is the role of probiotics.
I’ve got a huge list of reasons why you need to get more probiotics in your diet.
Probiotics can be life-changing for people who have been suffering for years. You’ll be surprised at the range of symptoms that are caused by a simple lack of enough — or the right kind of — probiotics!
But first, here's a recap of what probiotics are and what they do.
What Are Probiotics
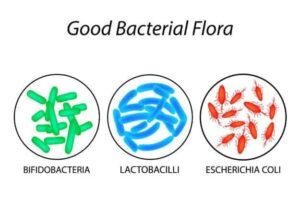
Probiotics are the “good” or “friendly” bacteria in the GI tract. They are markers for good digestive health.
A healthy adult human should be host to 3-5 pounds of these microbes (at least 70 trillion — more bacterial cells in the host than actual DNA-containing cells).
Probiotics are the “good” or “friendly” bacteria in the GI tract. They are markers for good digestive health.
Probiotics are vital to support the immune system, brain and mood function, and absorption of food and nutrients. They control inflammation, trigger hormone production, and remove waste.
Dr. Bernard Jensen | GI Tract Study
One of my heroes, Dr. Bernard Jensen, was a pioneer in GI tract health.
He studied 10,000 people’s colons and noted that the healthiest people had far more beneficial bacteria than the “bad,” like communicable disease germs such as strep and staph.
At that time, 30 or more years ago, he reported that Americans’ good-to-bad ratios were far too low. Since then, our ratios have gotten even worse, leading to more and more diseases.
That’s because many aspects of modern life are hostile to the good gut microbes, and even encourage the growth of the bad ones.
How Do You Know You Have Enough Good Bacteria
There are lots of reasons that you might struggle to have enough good bacteria in your system.
Most are things you can control, but others are out of your hands.
That’s why you should know what the signs of bacteria imbalance are, and what to do about it.
The foods we eat, the medicines we take, the toxins we’re exposed to, stress levels, and even how we’re born all affect which microbes flourish and which ones struggle.
Do You Need Probiotics?
There is no easy, reliable way to “measure” your gut bacteria ratios, but there are some tell-tale signs, situations, and symptoms that probably mean you should take steps to increase the “good guys” column in the balance sheet (more on how to do that later).
You should actively boost your probiotics if:
1. You Have Used Antibiotics

Ever. Even once. Even decades ago.
The “anti” of “antibiotics” means that these drugs are not selective when it comes to killing off bacteria. The good probiotics are wiped out along with the bad, but then a vicious cycle can start.
Probiotics are essential for immune function, so a gut wiped out by antibiotics can’t defend you against bugs like the flu strep, or staph. And what is prescribed for strep and other infections? Yep. More antibiotics.
The Side Effects of Antibiotics
Some care standards even require doctors, dentists, or other health professionals to administer antibiotics “proactively.”
I’ve questioned that practice before, and my reasons still stand: I used to get strep as a kid, several times a year. I believe that so many courses of antibiotics destroyed my immune system, and it took me years of good nutrition to recover.
Resistance to Antibiotics
And of course, the consequence of the “preventative antibiotics” trend is MRSA infections and many other “superbugs” that are antibiotic-resistant, plus a host of yeast problems and gut issues related to all the natural flora being destroyed in the gut from even one dose of antibiotic.
And the longer it goes on, the worse it can get. (I wrote about Allie’s horrific story of antibiotic-induced hell, and how she dug herself out of it.)
Restore Your Good Bacteria
The kicker? If you’ve taken antibiotics, your store of good bacteria does NOT recover naturally.
You have to consciously take steps to replace them and restore a healthy balance.
The key is to strengthen and support gut health.
2. You Have Digestive Issues
Abdominal pain is the number one symptom of insufficient probiotics. A primary role of beneficial bacteria is to break down food for absorption.
Symptoms of Probiotics Deficiency
When food isn’t broken down properly, you can get any of several symptoms:
- Acid Reflux, Heartburn, and Ulcers: Without enough probiotics in the upper GI tract, you can suffer an overrun of bad bacteria such as H. Pylori, a microbe which can cause sores serious enough to lead to cancer.
- Bloating: Undigested food can begin to ferment in the intestines, and a byproduct of fermentation is gas. The gas swells the intestines where it is trapped, causing pain and bloating as it moves through the twists and turns.
- Flatulence: Undigested, fermenting food not only produces gas (which eventually needs to escape somewhere); it can also be extra smelly as the undigested food begins to putrefy.
- Constipation: The colon is the final chance for probiotics to do their job. If you’ve starved them of the fiber they live on, you’ll have too small of a colony to keep your stools soft and moving.
- Irritable Bowel Syndrome: The most common GI disorder in the world, this painful disease is related to constipation and other bowel issues, and the latest studies show probiotic therapy to be useful.
- Diarrhea: One job of colon microbes is to reabsorb water from the stool as it passes through. If an infection (or antibiotics) has wiped the microbes out, too much water is left in the colon, and it passes as diarrhea, putting you at risk for dehydration.
3. You Catch Every Bug That Goes Around
The Human Microbiome Project has spent millions of dollars to catalog “microbiome communities” in people with different diseases.
The more data mounts, the clearer it becomes that a varied and healthy gut population has everything to do with a strong immune system and resistance to disease, including cancer.
How Probiotics Strengthen Immunity
Beneficial bacteria tackle all the different kinds of invaders that come into your body through all the different channels — breathing, touching, eating, sexual contact, etc.
Bacteria have specialized jobs that vary from strain to strain, and they work to fight the baddies in different ways. Some of those jobs include:
- Crowding out invaders by sheer number, keeping them from feeding and multiplying.
- Strengthening and guarding gut and other cell linings, only allowing molecules they recognize to get through.
- Regulating the inflammatory response to attack pathogens, without going overboard and attacking your own systems and resulting in allergic or autoimmune disorders.
- Maintaining pH levels that are inhospitable to infectious bacteria.
- Being “support staff” to other good bacteria, keeping them fed or carrying off their waste.
- Breaking down foods into nutrients the body can use to create white blood cells and repair damage.
4. You Eat Toxic Food, Including Sugar
The Standard American Diet includes “foods” that would upset microbial balance on their own, but the combination common to most SAD eaters is truly toxic.
They include:
- Sugar: Sugar of any kind feeds bad bacteria and yeast organisms, all of which can quickly overwhelm a gut biome too low on the probiotics to fight them.
- Processed Food: Processed food, with low-to-no natural fiber, feeds only the beneficial bacteria in the upper GI tract. It is digested before it hits the large intestine, starving the beneficial bacteria there and setting you up for colon disorders and disease.
- Artificial Sweeteners: Besides being neurotoxic, artificial sweeteners have been shown to increase the bacteria associated with glucose intolerance and Type 2 diabetes.
- GMOs: Hybridized grains have been linked with the pain and inflammation of “leaky gut,” by damaging the bacteria that are responsible for maintaining the gut lining.
- Fast Food: The meats and fried foods common to fast food restaurants feed bad bacteria and starve the good bacteria of fiber and prebiotics that they need to live on.
- Over-The-Counter Medications: Anti-inflammatories such as ibuprofen and acetaminophen are highly damaging to gut linings and the beneficial bacteria that live there.
5. You are Depressed, Anxious, Stressed, or Have Other Mood, Memory, or Cognitive Symptoms
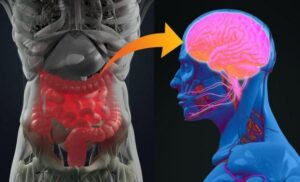
Some of the most exciting studies released recently show that mental health is closely related to gut health. In fact, the link is so strong that it’s being called the “gut-brain axis.”
Probiotic Benefits for the Brain
Serotonin and other neurotransmitters responsible for feelings of well-being are profoundly influenced by any changes in your microbiome.
In fact, 90% of your body’s serotonin is produced in your gut!
The gut and brain communicate with each other via the vagus nerve, a cranial nerve that runs from the brain stem down to the abdomen. When the brain senses enough serotonin in the gut, it lowers stress hormones like cortisol, helping you feel more calm, relaxed, and content.
The effects go far beyond stress. A 2017 metastudy showed improvements in symptoms of depression, anxiety, and memory loss after participants took sufficient levels of probiotics.
[Related: How To Fight Depression and Anxiety: 12 Nutrition Strategies]
6. You Were Born via Cesarean Section
The makeup of your gut microbiome is “hereditary,” meaning that most of the bacteria are passed from mother to baby during a vaginal birth (just as it was passed to the mother from her mother).
Babies born vaginally have a much richer variety of bacteria in the weeks immediately following birth than those arriving via the more sterile environment of a C-section.
Avoid Neonatal Probiotic Deficiency
This early biodiversity can mean better long-term outcomes. A C-section baby can catch up if parents are diligent about making sure the baby gets enough probiotics through breastfeeding or supplemented formula.
7. You Can’t Sleep
It turns out that your gut health has a lot to do with how restfully you sleep.
Remember that “gut-brain axis"? Your microbiome is responsible for making the amino acid tryptophan, a precursor to sleep cycle-regulating hormones, serotonin and melatonin.
If your gut microbes don’t have enough diversity or numbers to produce sufficient tryptophan, your brain can’t relax and turn off thoughts for the night.
Of course, the serotonin itself is important for sleep as it prevents disorders like depression and anxiety that tend to disrupt sleeping patterns.
Production of the Amino Acid GABA
Your gut is also responsible for producing GABA, an amino acid that is essential for restorative sleep.
GABA works to calm the central nervous system, and even quiets various forms of pain that can keep you from getting enough z’s.
Making sure you get enough probiotics during the day will make all the difference at night.
8. You’re Gaining Weight
Weight loss promises are always a big draw, and diet fads come and go while people look for the next big thing.
But managing your weight could be as simple as making sure you get enough probiotic-rich food!
Benefits of Probiotics for Weight Loss
Though researchers are just in the beginning phases of understanding how the gut microbiome affects things like fat metabolism and body mass, it’s clear that it does play a role.
A recent study showed that probiotics signal the body to break down fat into forms that cells can use for energy, instead of just storing the fat intact. Probiotics “reduced the body weight, body fat percentage, body fat mass and subcutaneous fat area in overweight subjects.”
[Related: How to Change Your Weight “Set Point” Forever]
9. You Have Acne, Rosacea, Eczema, or Other Skin Disorders

Your skin is home to its own colonies of bacteria. In fact, the skin has its own microbiome, science is discovering.
So healthy, clear skin relies on maintaining good bacteria, both inside and out.
Here’s what we know about three common skin conditions and how probiotics can help:
- Acne: One common cause of acne is a particular group of bacteria, so it has often been treated with antibiotics to kill them (which unfortunately kills all the good bacteria, too). Some bacteria produce antimicrobials helping skin clear from within. New probiotic treatments to apply directly to the skin are promising, as well.
- Rosacea: As with acne, rosacea flare-ups are complex, and there are several ways that oral or topical probiotics can help: as a protective, antimicrobial shield if used topically, and as a stress-calmer and inflammation-tamer when taken orally.
- Eczema: Studies on infants at risk for eczema have shown that when the mother takes probiotics before and after birth, the babies have a more diverse microbiome, and are less likely to develop eczema.
[Related: 7 Key Nutrition Factors for Youthful Beauty You Will Love]
10. You Don’t Eat Your Veggies
It’s all about fiber! Fiber from whole grains, fruits, and vegetables are not actually digested by humans. It’s food for the billions of friendly bacteria that live in your colon.
It’s a symbiotic relationship—you feed the colon’s bacterial colony, and they take care of you in countless ways.
Fiber also provides bulk to move wastes through the colon and out of your body. It holds enough water to keep stools soft and avoid constipation.
11. You are Over the Age of 40
Aging bodies have a harder time maintaining the balance of beneficial versus harmful gut bacteria.
The growing imbalance leads to deteriorating gut linings, susceptibility to disease, and increasing inflammation (which speeds up aging).
People over 40 need to be deliberate and diligent about making sure they get lots of probiotics in their diets. They should take supplements as well.
How Do You Get Enough Probiotics?
Helping people heal their gut with whole foods has been a passion of mine from day one; there's an entire chapter in 12 Steps to Whole Foods to educate people, and I’ve got a Video Masterclass series on the topic as well.
Here are the ways I suggest making sure you get enough probiotics, daily:
1. Eat Cultured Foods
Are you scared of fermented food? Cultured and fermented foods are part of your diet already if you eat yogurt or sauerkraut or kefir. Every culture in the world eats cultured foods.
My work focuses on culturing vegetables, optionally some raw, antibiotic- and hormone-free milk, or coconut liquid. In fact, I now culture my coconut liquid before using it in Hot Pink Breakfast Smoothie, which is one of my most-loved recipes in the 12 Steps course where we shift to whole-foods breakfasts.
Eat Unprocessed Foods
Yogurt always comes up when discussing cultured foods. Make sure you skip the fake flavorings and sweeteners. And if you’re buying pasteurized stuff, the cultures are likely already dead. Try making your own, with raw, hormone-free milk.
Check out my Facebook Live where I ate 10-year old RAW cabbage… and lived to tell about it! We talked about the importance of fermented and cultured food, and getting over the fear of both making and eating them!
Homemade Kefir Probiotic
You can also make your own kefir. It’s a cheap and easy way to rehab and strengthen the microbiome that gives you more diversity in healthy microbes than yogurt does.
I have an entire Rehab Your Gut With Food video in the 12 Steps to Whole Foods Video Masterclass to learn more.
2. Take Probiotic Supplements
Not all probiotic supplements are created equal!
Twenty years ago, the first probiotic supplements were just acidophilus, or perhaps two or three strains.
Then, we learned that there are actually hundreds of strains of healthy bacteria in the human gut.
The more variety, the better, for colonizing a strong microbiome.
Look for a supplement that has:
- At least 10-15 strains of probiotics (the more, the better!): Since different bacteria do different jobs, you need a broad diversity of types to strengthen and colonize your gut.
- Fresh ingredients with live cultures: Many probiotic supplements have been in the supply chain too long, and the cultures are old and dead. In a recent Facebook Live video, I show you an at-home experiment to do overnight that will show you if your probiotic is still viable.
- An added prebiotic: Prebiotics feed probiotics, increasing their number and optimizing their ability to do their work in the gut.
- Digestive enzymes: Good digestion also requires enzymes in your diet. Enzymes break down proteins, fats, and carbs, these nutrients so they can be better used by your gut flora, as they travel through the digestive tract.
(Since I couldn’t find a probiotic supplement that fit all those requirements, I researched and made my own, so we could have live cultures, made in small batches for freshness. Check out PreZyme Pro in the GSG store!)
[Related: How to Test Your Probiotic Supplement: An Easy At-Home Experiment]
The good news is that getting and maintaining a good gut bacteria balance is completely doable. Knowing where you’re at risk, and what to do about it, are important first steps.
Ready to learn more?
Watch my 12 Steps to Whole Foods Video Masterclass, which is currently free!
Learn how to heal your gut with just 10 cents per day, which foods fight inflammation, how to beat your food addictions, and more!

Disclosure: This post may contain affiliate links that help support the GSG mission without costing you extra. I recommend only companies and products that I use myself.

Sources
- Leone, V., Gibbons, S., Martinez, K., Hutchison, A., Huang, E., Cham, C., Chang, E. (2015). "Effects of Diurnal Variation of Gut Microbes and High-Fat Feeding on Host Circadian Clock Function and Metabolism." Cell Host & Microbe, 17(5), 681–689.
- Nakamaru-Ogiso, E., Miyamoto, H., Hamada, K., Tsukada, K., & Takai, K. (2012). "Novel biochemical manipulation of brain serotonin reveals a role of serotonin in the circadian rhythm of sleep-wake cycles." European Journal of Neuroscience, 35(11), 1762–1770.
- Owens MJ, Nemeroff CB. "Role of serotonin in the pathophysiology of depression: focus on the serotonin transporter." Clin Chem. 1994;40(2):288–295. [PubMed]
- X. Hébuterne. "Gut changes attributed to aging: effects on intestinal microflora." Curr Opin Clin Nutr Metab Care, 6 (2003), pp. 49-54
Posted in: Immunity, Supplements, Tools & Products, Whole Food
















Dear Robyn
thank you so much,I know more than before on probiotics,I appreciate it,all my best to you ,Luisa
I don’t believe and promote PRObiotic. Supplements are not the way to good health. People needs to EAT their food, and fruits and veggie are loaded with soluble fiber (Prebiotic) for our microbiome. So your green smoothies are good source.
You don’t believe and promote Probiotics? Exactly what kind of doctor are you? lol
My colon was removed 12 months ago, is this type of fetox suitable for me
Luisa, thank you for writing and sharing!
Are there any other brands of probiotics that you would recommend particularly for a 4 year old (chewable or otherwise easy to take?)
Thank you!
Is there any specific time to take probiotics?
Hi Akki, for our PreZyme Pro, the suggested use is as follows: One capsule, twice daily, just prior to or with meals. And for added support we suggest you eat cultured foods through the day, such as real yogurt, sauerkraut or kefir.
In case you missed it, here’s the link to our GSG PreZyme Pro: https://shop.greensmoothiegirl.com/products/prezyme-pro
A lot of these links are broken or lead to pages that have no relevance to the topic.
I tried to access your link to “alternatives to antibiotics” and it didn’t work. Is there another way to get that information?
Your links to "alternatives to antibiotics" and "own kefir" don’t work.